About our Department
Our research
Our Research
The Department of Radiotherapy at the Erasmus MC Cancer Institute is committed to research for the betterment of clinical care. Completed research is often followed up by clinical implementation and novel strategies are tested in clinical trials. Since 2018, the department has moved to a new building with state-of-the-art radiotherapy equipment at Erasmus MC’s central campus in Rotterdam. The department is also strongly involved in the research and patient treatments in the Holland Proton Therapy Center in Delft.
Clinical Research
Clinical research includes the development of clinical trials testing new treatment techniques for the reduction of radiation-induced side effects, and the creation of prospective cohort to capture the long-term radiation outcomes. Those cohorts will enable the development of predictive toxicity models and to test prevention strategies. They will also permit the discovery of mechanisms involved in toxicity or the prolonged survival after ablative treatment for oligometastatic patients.
Medical Physics and Technology
The Department of Radiotherapy at the Erasmus MC Cancer Institute has been at the forefront in developing automated treatment planning and high-precision adaptive radiotherapy approaches. This includes online and even real-time adaptive radiotherapy, robotic stereotactic body radiotherapy and proton therapy. Other focus areas are biology image-guided radiotherapy, and technology for interventional radiotherapy such as brachytherapy and hyperthermia. An important goal of the research program is to implement completed research and to evaluate the benefit.
Radiobiology Research
This covers research on the fundamental mechanism of the DNA damage response, specially damage induced by radiation. Understanding those mechanisms leads, beyond the mechanistic understanding, to the design of novel targeted approaches, including those modulating the DNA damage response such as hyperthermia or small molecule inhibitors, to increase the therapeutic windows between rapidly replicating cancer cells and normal tissues. It also leads to individualized radiation dose prescription if the tumor response to therapy of a given patient could be established based on radio- and thermo-biological molecular markers.Principal Investigators
Alejandra Mendez Romero, PhD MD
Ben Heijmen, Prof PhD
Dik van Gent, PhD
Dirk de Ruysscher, Prof PhD MD
Femke Froklage, PhD MD
Henrike Westerveld, PhD MD
Inger-Karine Kolkman-Deurloo, PhD
Jeremy Schiphof-Godart, PhD
Jeroen Essers, PhD
Joost Nuyttens, PhD MD
Jos Elbers, PhD MD
Joyce Lebbink, PhD
Kelvin Ng Wei Siang, PhD
Linda Rossi, PhD
Luca Incrocci, Prof PhD MD
Maaike Milder, PhD
Maarten Dirkx, PhD
Marta Capala, PhD MD
Martine Franckena, PhD MD
Michiel Kroesen, PhD MD
Miranda Christianen, PhD MD
Mischa Hoogeman, Prof PhD
Patrick Granton, PhD
Remi Nout, Prof PhD MD
Roland Kanaar, Prof PhD
Sebastiaan Breedveld, PhD
Sergio Curto, PhD
Steven Petit, PhD
Wilma Heemsbergen, PhD
Yvette Seppenwoolde, PhD
Research Lines
Research Lines
Research at the Department of Radiotherapy at the Erasmus MC Cancer Institute is demarcated into three distinct domains/groups, these being:
- Clinical research
- Medical Physics and Technology
- Molecular Biology
Clinical Research
Clinical research is initiated by research-driven scientists and supported by the clinical outcome unit, which is managed by René Vernhout and several staff.
The Clinical Outcome Unit enables the collection of prospective patient's data including well-defined pathology, various treatment modalities and highly specific endpoints (e.g. breast cardio-toxicity, prostate patients reported quality of life outcome).
Most important of all, the Clinical Outcome Unit facilities the running of clinical trials.
Medical Physics and Technology
A significant component of the department of radiotherapy at the Erasmus MC Cancer Institute is actively involved the technological aspects of clinical care. Due in part because treatments involve sophisticated devices with evolving complexities, it is important that management of these devices is maintained with sufficiently trained persons (i.e. Clinical Physicists, Engineers) and ensure that the quality of treatment remains high for good clinical care.
Frequently, new developments become available that offer improvements to the standard of care, and since it is the departments desire to be at the forefront of the medical advancements, adequate resources are required to ensure a smooth transition from the development phase of new technologies to clinical rollout.
Radiobiology Research
Radiobiology research is conducted alongside the Genetics Department.
This subdivision in these three research lines fails to capture, however, that a lot of our research increasingly takes place across these three domains. Therefore, the current research activities of the department has been classified into a number of research topics.
The research topics, grouped according to the research lines, are:
Clinical research
Prof. dr. R.A. Nout, Prof. dr. L. Incrocci, Prof. dr. D.K.M. de Ruysscher, Dr. A.M. Mendez Romero
Dr. M.E. Capala, Dr. M.E.M.C Christianen, Dr. J.B.W. Elbers, Dr. M. Franckena, Dr. E.A.M. Froklage, Dr. W.D. Heemsbergen, Dr. M. Kroesen, Dr. J.J.M.E. Nuyttens, Dr. M.J.J. Olofsen-van Acht, Dr. G.A. Sattler, Drs. G.M. Verduijn, Dr. H. Westerveld
o Gynaecological cancer
Optimizing radiotherapy of gynaecological tumours, including image guided adaptive radiotherapy for external beam and brachytherapy, international collaborative prospective studies, combined modality treatment, prediction modelling, development of proton therapy, translational research including immune radiotherapy interaction.
o Liver cancer
Research on clinical and technical aspects of stereotactic body radiotherapy treatments of tumours in the liver.
o Brain cancer
Research on clinical and technical aspects of proton therapy for low grade glioma’s; use of functional MR Imaging (MRI) for target delineation for brain tumours.
o Head and neck cancer
Research on improving and validation of the treatment of head and neck cancer, including prediction modelling, biologically adaptive radiotherapy, hypofractionation, immune radiotherapy interaction.
o Breast cancer
Research on improving and validation of the treatment of breast cancer, including optimizing treatment planning, prediction modelling, increasing tailored treatment by means of assessing 1) tumour and healthy tissue response prediction and 2) new multimodality approaches clinical studies in the neoadjuvant setting.
o Urological cancer
Research on hypofractionation and online adaptive radiotherapy, analysis of secondary tumours, and brachytherapy.
o Lung cancer
Research clinical and technical aspects of Stereotactic Body Radiotherapy (SBRT) treatments for primary tumours and oligo metastasis; personalized combined modality treatment.
Medical physics and technology
Prof. dr. M.S. Hoogeman, Prof. dr. B.J.M. Heijmen, Prof. dr. ir. M.M. Paulides, Dr. S.F. Petit
Dr. S. Breedveld, Dr. S. Curto Ramos, Dr. M.L.P Dirkx, Dr. P.V. Granton, Dr. M.T.W. Milder, Dr. I.K.K. Kolkman-Deurloo, Dr. J.J. Penninkhof, Dr. L. Rossi, Dr. J. Schiphof-Godart, Dr. Y. Seppenwoolde
o Treatment planning development
Research on multi-criteria decision making in (automated) treatment planning, real-time treatment plan generation, exploration and validation of novel treatment planning approaches.
o Applied treatment planning
Use of automated treatment planning for development, comparison and validation of treatment strategies in external beam photon radiotherapy.
o High-precision adaptive radiotherapy
Development and validation of methodologies for high-precision and anatomical adaptive radiotherapy with photon beams (C-arm linear accelerators, CyberKnife, and Ethos, incl. one-stop-shop, re-planning, imaging).
o Physics and technology for proton therapy
Physics and technology research in proton therapy, including robust evaluation and optimization, high-precision adaptive proton therapy, automated treatment planning, FLASH proton therapy, RBE/LET evaluation
and optimization, ocular beam proton therapy.
o Brachytherapy development
Technological development of Brachytherapy, including individualized applicator design, automated treatment planning, electro-magnetic catheter tracking.
o Technology and clinical application of hyperthermia
Applicator development, specific-absorption-rate/temperature optimization, thermometry based on Magnetic Resonance (MR), clinical implementation and evaluation.
Molecular radiation biology
(collaboration with the department of Molecular Genetics)
Prof. dr. R. Kanaar, Dr. J. Essers, Dr. D.C. van Gent, Dr. J.H.G. Lebbink
Dr. M.E. Capala, Dr. M.P. Chien, Dr. A. Ray Chaudhuri, Dr. N. Taneja, Dr. A. Zelensky
o Molecular Mechanisms of the DNA Damage Response
Aims to address fundamental molecular mechanistic aspects of the DNA damage response, in its broadest sense, by pursuing complementary and interwoven approaches at both the molecular and cellular level.
o The DNA Damage Response in Cancer
Aims to provide a rational basis for improving existing approaches and developing entirely novel and innovative precision therapies for cancer and aging-related diseases. To bring to the clinic better criteria and tools for individual patient selection for precision therapy in the context of cancer. To develop reliable prognostic tools for treatment of cancer and aging related diseases.
Projects
Publications
Facilities
The department of Radiotherapy within the Erasmus MC Cancer Institute in Rotterdam includes the satellite treatment center next to the Albert Schweitzer Hospital in Dordrecht.
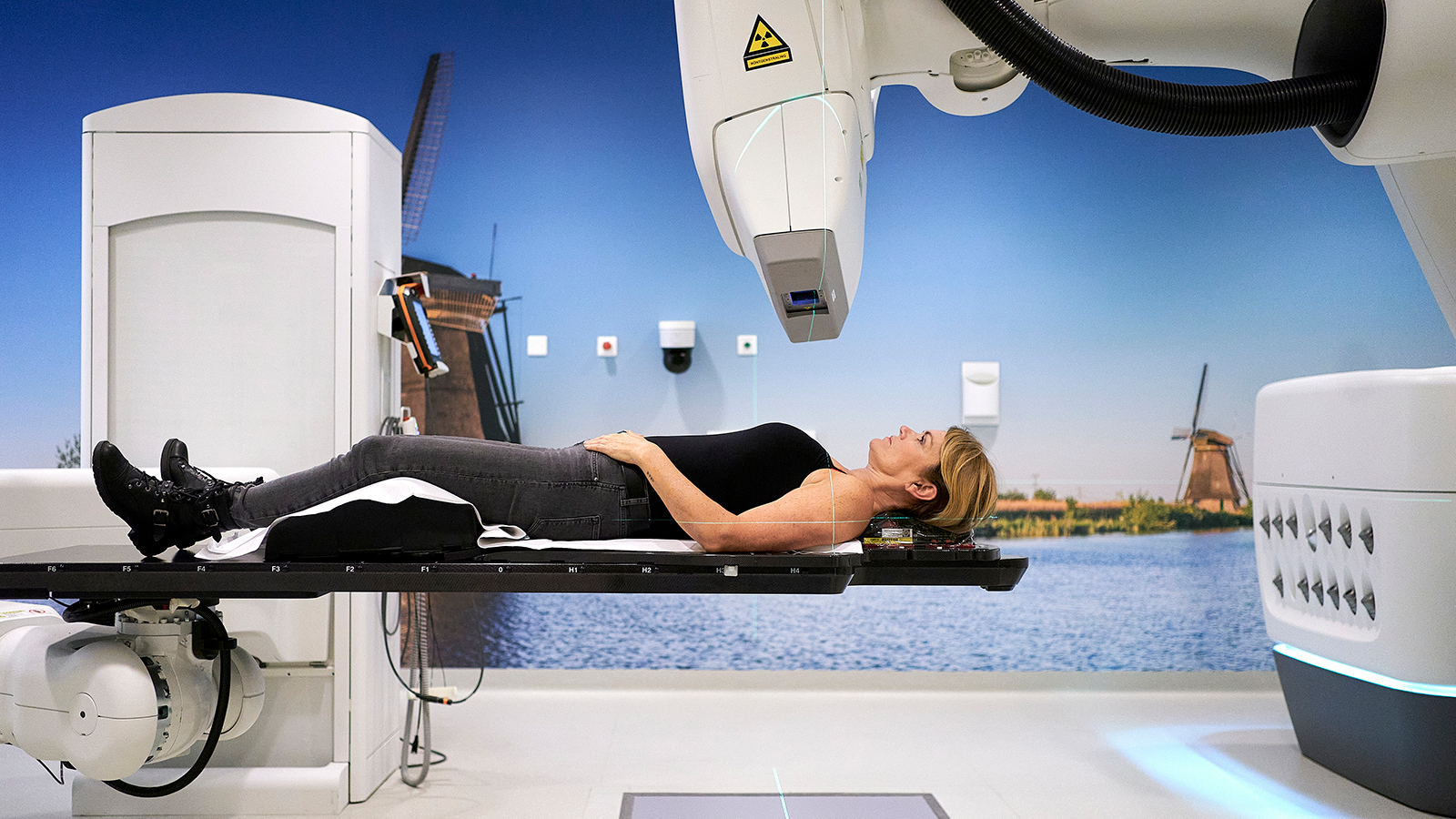
Cyberknife
Together with Dordrecht, the department manages ten Elekta Linacs (six Versa HD, four Agility), six surface guidance devices, two Cyberknifes (one with an in-room CT on rails), two brachy Afterloaders, three planning CT machines, and two hyperthermia devices (one for deep seated tumors like the cervix, and the other for targets within the head and neck region).
In addition, the department has shared resources with the radiology department including 1.5 and 3 T MRI scanners as well as PET scanner in the nuclear medicine department.
The department of Radiotherapy at Erasmus MC, together with the centers of TU delft and Leiden MC, equally founded HollandPTC - an independent outpatient center for proton therapy, scientific research and education, located in Delft.
Collaborations
Collaboration within Erasmus MC
- Department of Otorhinolaryngology
- Academic Center of Excellence for Genito-Urinary Tumors
Outside Erasmus MC Cancer Institute
- NVKF Nederlandse Vereniging voor Klinische Fysica
- NVKFM Nederlandse Vereniging Klinisch Fysisch Medewerkers
- NVRO Nederlandse Vereniging voor Radiotherapie en Oncologie
- ESTRO The European Society for Therapeutic Radiology and Oncology
- EORTC European Organisation for Research and Treatment of Cancer
Related departments
- Holland PTC Proton Therapy Centre Delft
- SBE Erasmus MC Radiation Protection